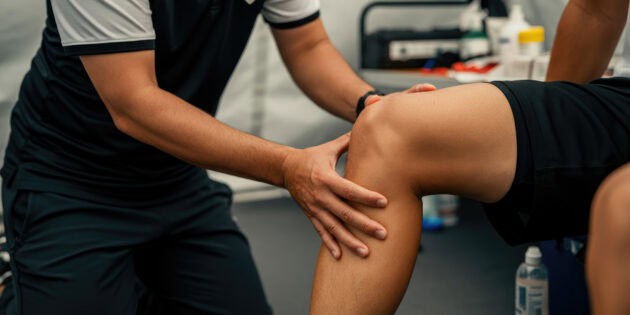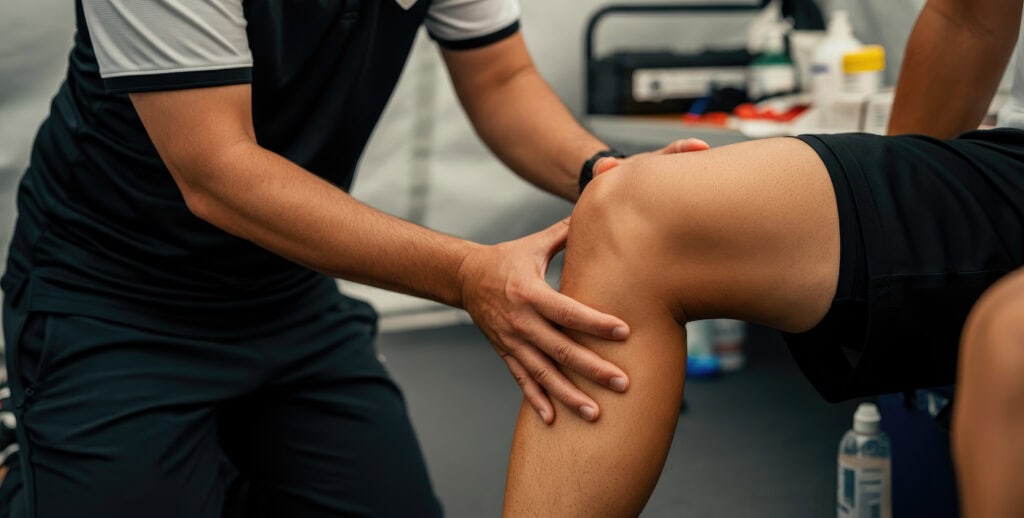
ACL reconstruction recovery takes 9 to 12 months for most athletes to safely return to full sport, though many people feel functionally normal well before that. Physical therapy begins within the first week of surgery and runs through six distinct phases over that period. The research is clear that athletes who rush this timeline have significantly higher re-tear rates — but those who follow a structured, criteria-based progression come back stronger than before.
ACL injuries have a way of stopping life in its tracks. One moment you are mid-run, mid-cut, mid-landing — and then there is a pop, and everything changes. The surgery itself is almost the easy part. It is the nine to twelve months that follow where most of the real work happens.
I have worked with a lot of ACL patients over the years, across all ages and sports. High school athletes who tore their ACL during football season and want to be back on the field for spring. Recreational soccer players in their 30s and 40s who want to return to their weekend league. Avid hikers and trail runners in Orange County who just want to get back on the trails without their knee giving way.
What they all have in common is this: they want to know exactly what the recovery looks like, what the milestones are, and what they need to do to get back to full function as safely and efficiently as possible.
That is what this article is for. I want to give you an honest, detailed picture of ACL recovery — week by week, phase by phase — so you understand what your body is doing at each stage and what good rehabilitation looks like throughout.
Table of Contents
What Happens During ACL Reconstruction Surgery?
The ACL — anterior cruciate ligament — is one of the four main ligaments stabilizing the knee joint. It runs diagonally through the centre of the knee and controls rotational stability and forward movement of the tibia. When it tears, the knee loses that control, which is why it buckles or gives way under load.
ACL reconstruction replaces the torn ligament with a graft — tissue taken from elsewhere in your body or from a donor. The three most common graft options are the patellar tendon (bone-patellar tendon-bone), the hamstring tendon, and the quadriceps tendon. Each has different characteristics in terms of initial strength, healing biology, and donor site recovery, and your surgeon will have chosen based on your age, activity demands, and anatomy.
The graft is threaded through tunnels drilled into the femur and tibia and secured in place. Over the following months, a biological process called ligamentisation gradually transforms the graft into functional ACL tissue. This process — not just the surgical healing — is what dictates the recovery timeline. The graft looks like an ACL relatively quickly. It takes much longer to behave like one under the stresses of sport.
When Does Physical Therapy Start After ACL Reconstruction?
Physical therapy begins within the first week of surgery — often within the first two to three days. Early movement is essential. Research consistently shows that patients who begin PT early after ACL reconstruction regain range of motion faster, reduce swelling more effectively, and have better functional outcomes at six months compared to those who wait.
The immediate priorities are straightforward: regain full knee extension (complete straightening), control swelling, activate the quad, and restore a normal walking pattern. None of this sounds dramatic, but each of these early goals has a direct downstream effect on how the later phases of recovery unfold.
One note for athletes who had a concurrent meniscus repair: the timeline changes. Meniscus healing adds constraints to early weight bearing and range of motion work, and the overall recovery is typically longer. Your PT will know this and adjust the program accordingly.
ACL Recovery Timeline Week by Week
ACL rehabilitation moves through six phases. The transition between phases is criteria-based — meaning you move forward when your knee is ready, not simply when the calendar says so. This is one of the most important things to understand about ACL recovery. Time is a guide, not a gate.
Phase 1 — Weeks 1 to 2: Control Swelling, Restore Extension, Wake Up the Quad
The first two weeks set up everything that follows. Swelling needs to come down, the knee needs to straighten fully, and the quad — which shuts down almost immediately after ACL surgery — needs to start firing again.
Quad sets, straight leg raises, heel slides, and prone hangs for extension are the foundation of this phase. They feel almost insultingly simple for an athlete. They are not. A quad that does not activate properly in week one creates compensatory movement patterns that cause problems months later.
Most patients are walking with crutches at this stage, transitioning to full weight bearing as the quad strength and pain allow. Goal by end of week two: full knee extension matching the other side, at least 90 degrees of flexion, and controlled quad activation.
Phase 2 — Weeks 2 to 6: Restore Range of Motion and Build Early Strength
Full weight bearing is established. The crutches are gone or nearly gone. Range of motion work continues, with the goal of reaching 130 degrees or more of flexion. Strengthening progresses to closed chain exercises — mini squats, leg press, step-ups — which are safer for the healing graft than open chain movements at this stage.
Gait retraining is a priority. Many patients develop a subtle limp or quad avoidance pattern that sticks around long after the pain is gone. Catching and correcting this early prevents it from becoming a habit that undermines the whole recovery.
Hip and glute strengthening starts here too. The hip controls the knee from above, and weak glutes are a contributing factor in ACL re-tears. Building hip strength early is not optional — it is part of building a knee that holds up under load.
Phase 3 — Weeks 6 to 12: Progressive Strengthening and Neuromuscular Control
This is where the training load increases meaningfully. The graft has initial structural integrity, though ligamentisation is still in its early stages. Exercises progress to include single leg work, Romanian deadlifts, lateral movements, and balance training on unstable surfaces.
Neuromuscular control — the ability of the nervous system to coordinate muscle activation around the knee in real time — is a major focus of this phase. This is what protects the knee when the ground shifts unexpectedly, when you cut without thinking about it, when the sport demands more than a controlled gym environment. Training it takes time and repetition, and it cannot be shortcut.
Strength testing typically happens around the 12-week mark. Limb symmetry index — a comparison of the surgical versus non-surgical leg — is the benchmark. Most programs require 70 percent symmetry before progressing to the next phase.
Phase 4 — Months 3 to 6: Running, Agility, and Sport-Specific Preparation
For most athletes, this is the phase they have been waiting for. Running returns — but through a structured progression, starting with straight-line jogging and building gradually to faster running, lateral movement, and direction changes.
Agility drills, cutting patterns, deceleration training, and sport-specific movement are introduced progressively through this phase. Plyometrics — jumping, landing, bounding — begin conservatively and build toward the demands of your specific sport.
This is also the phase where athletes tend to feel normal and want to jump ahead. The knee feels fine. The swelling is gone. The strength feels close to what it was. But the graft is still in the middle of ligamentisation — it is at its weakest relative to its structural appearance around month four to six, which is exactly when re-tears most commonly happen in athletes who return to sport too early.
Phase 5 — Months 6 to 9: Return-to-Sport Testing and Progressive Exposure
Return to sport is not a date on a calendar. It is a series of criteria that need to be met — and the research is unambiguous on this. A 2016 meta-analysis published in the British Journal of Sports Medicine found that athletes who met strength and functional criteria before returning to sport had a five times lower re-tear rate than those who returned based on time alone.
At Intecore, the criteria we use include achieving 90 percent or greater limb symmetry on strength testing, passing hop tests on the surgical leg, demonstrating controlled landing mechanics under fatigue, and completing a full sport-specific movement battery without compensatory patterns.
Controlled return to sport begins here — practice before games, non-contact drills before full contact, monitored exposure before unrestricted play. Each step is earned, not assumed.
Phase 6 — Months 9 to 12: Full Return and Long-Term Resilience
Full unrestricted return to sport typically happens between nine and twelve months, once all criteria are met and the athlete has demonstrated they can handle the full demands of their sport without protective compensation.
The work does not end at return to sport. Ongoing strength and neuromuscular maintenance significantly reduces long-term re-tear risk and protects the other knee, which carries elevated injury risk for two years after ACL reconstruction. A good PT program addresses both knees during the later phases of recovery.
Does Graft Type Affect Recovery Timeline?
Yes, though the differences are often overstated. Here is a practical summary.
- Patellar tendon (BTB) graft: Considered the gold standard for high-demand athletes due to bone-to-bone healing and strong long-term outcomes. Donor site pain — in the front of the knee — can be significant in the first few months and requires specific attention in rehab.
- Hamstring graft: Less donor site discomfort than BTB, good outcomes across most patient populations. Hamstring strength deficits on the surgical side need to be addressed specifically in rehabilitation and are sometimes undertreated.
- Quad tendon graft: Growing in popularity, particularly for younger athletes. Large cross-sectional area and strong early fixation. Quad strength recovery in the early phase needs specific focus given the donor site location.
- Allograft (donor tissue): Longer ligamentisation timeline than autograft options. Generally not recommended for young, high-demand athletes due to higher re-tear rates in that population. May be appropriate for older, lower-demand patients.
Your PT should know your graft type and factor it into the programming. The broad strokes of rehab are similar across graft types, but the specifics of donor site management and loading progressions differ.
What Actually Slows Down ACL Recovery?
In my experience working with ACL patients in Southern California, the same factors show up repeatedly in the recoveries that stall or go backwards.
- Persistent quad weakness: The single biggest predictor of a slow recovery and elevated re-tear risk. Quad strength needs to be measured, tracked, and addressed aggressively throughout.
- Returning to running too early: Running before full extension, adequate quad strength, and normal gait mechanics puts load through a graft that is not ready for it. The knee may feel fine. The biology does not care.
- Skipping the psychological side: Fear of re-injury is a real and measurable barrier to return to sport. Athletes who score poorly on psychological readiness measures re-tear at higher rates, even when their physical criteria are met. This is something good PT addresses directly.
- Inadequate sleep and recovery: Tissue healing and neuromuscular adaptation happen during rest. Athletes who train hard but sleep poorly or under-eat consistently progress slower than those who treat recovery as part of the program.
- Treating criteria as optional: The timeline is a guide. The criteria are the gate. Returning to sport before meeting strength and movement benchmarks is the fastest route to a second ACL tear.
ACL Rehabilitation in Southern California
At Intecore Physical Therapy, we work with ACL patients across our clinics in Foothill Ranch, Aliso Viejo, and San Juan Capistrano. Athletes at every level — high school, recreational, competitive adult — come through our doors after ACL reconstruction, and the approach is the same for all of them: criteria-based progression, honest communication about where you are in the timeline, and a program built around getting you back to what you love doing.
We also work with athletes before surgery. If your ACL tear has been confirmed and a date is set, starting prehab now will give you a meaningfully better starting point on the other side of the procedure. The research on this is consistent — athletes who come in stronger go home stronger.
Fill out our quick inquiry form at intecorept.com/inquire or call us at (949) 597-2103. We will take a look at where you are and tell you exactly what the plan looks like from here.
Frequently Asked Questions
How long does ACL reconstruction recovery take?
Most athletes return to full unrestricted sport between nine and twelve months. Some reach that point closer to nine months, others take the full twelve or slightly longer — particularly those recovering from concurrent meniscus repairs or those returning to high-demand cutting and pivoting sports. The key is meeting criteria, not hitting a date.
When can I start running after ACL surgery?
Straight-line jogging typically begins around months three to four, once full range of motion is restored, quad strength is at least 70 percent of the non-surgical side, and gait mechanics are normal. Running before these criteria are met increases load on a graft that is still in its most vulnerable stage of ligamentisation.
What is the re-tear rate after ACL reconstruction?
Re-tear rates vary significantly based on age, sport, and whether a structured criteria-based return-to-sport protocol was followed. Young athletes under 25 returning to cutting and pivoting sports have the highest risk — some studies report re-tear rates of 15 to 25 percent in this group when return is time-based rather than criteria-based. Athletes who complete a full rehabilitation program and meet all return-to-sport criteria reduce that risk substantially.
Does ACL surgery recovery differ if I also had a meniscus repair?
Yes — meaningfully. Meniscus repair adds constraints to early weight bearing and range of motion work, typically extending the protected phase by several weeks. The overall recovery timeline is often 12 months or more when a significant meniscus repair is involved. Your PT needs to know the specific repair that was done and factor it into every phase of the program.
Should I do physical therapy before ACL surgery?
Yes. Pre-surgical PT — prehabilitation — consistently improves post-surgical outcomes for ACL reconstruction. Athletes who enter surgery with better quad strength, full range of motion, and normal movement patterns recover faster and achieve better functional results at six months. If your surgery is scheduled, contact us now to start a prehab program before your procedure date.
How do I know when I am ready to return to sport?
Readiness for return to sport is determined by a combination of strength testing (limb symmetry index of 90 percent or greater), functional hop testing, movement quality assessment, and psychological readiness. Feeling ready and being ready are not the same thing — and the gap between them is where most re-tears happen. Your PT should be running formal return-to-sport testing before clearing you for full sport, not making that call based on how you report feeling.
Sources
Here’s the sources section ready to paste into WordPress:
Sources
- Spinal Fusion Recovery: A Realistic Guide to the Timeline, the Restrictions, and the Role of Physical Therapy - April 8, 2026
- Hip Replacement Recovery: A Realistic Week-by-Week Guide for Southern California Patients - April 8, 2026
- ACL Reconstruction Recovery: A Realistic Week-by-Week Rehab Timeline for Southern California Athletes - April 7, 2026